Implant and Surgical
Extractions
When tooth extraction is needed: Generally, we recommend treatments that will save teeth, but when a tooth is so damaged that it cannot be saved, extraction is the best choice. Extraction might be best for:
- Teeth that are fractured below the gumline
- Severe tooth decay
- Advanced periodontal disease
- Primary teeth that are too crowded or not falling out properly
- An impacted wisdom tooth
The Procedure
Before we start the extraction procedure, we may offer nitrous oxide to relax you, and we’ll numb the area with anesthetic to keep you comfortable. After several minutes, we check the area to make sure that it’s completely numb. During the procedure, you’ll feel pressure when the tooth is removed, but you shouldn’t feel any pain at all. If you do, we’ll stop and give you more anesthetic.
Sometimes, if you tooth’s roots are curved or are held tightly in the socket, it’s helpful to cut the tooth into sections before removing them. If an incision was necessary, we may close it with a couple of stitches once the tooth is removed.
Taking care of yourself after the extraction:
To minimize problems after your tooth is removed, you’ll need to follow our post-operative instructions carefully, especially for the first 24 hours. These instructions will explain how to control bleeding, how to relieve pain and minimize swelling, how to prevent dry socket, and what to eat and not eat.
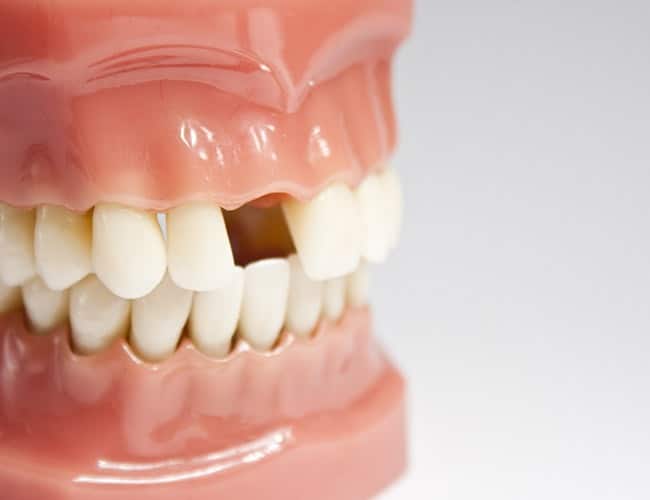
Why missing teeth need to be replaced
Teeth need each other for support. When you lose a tooth, the biting forces change on the teeth next to the space, causing the teeth to shift. In addition, the opposing teeth no longer have anything to chew against, so they may begin to extrude out of their sockets. These changes create places around the teeth that are hard to keep clean, so plaque and bacteria accumulate quickly. This accumulation can cause tooth decay and periodontal disease.
Changes in the bite can also put improper chewing forces on the shifted teeth, and this can lead to loose teeth and loss of jawbone, especially when periodontal disease is already present in your mouth. An uneven bite makes it harder to chew your food and may lead to grinding and clenching. A bad bite can also create painful problems with your jaw joint, the TMJ.
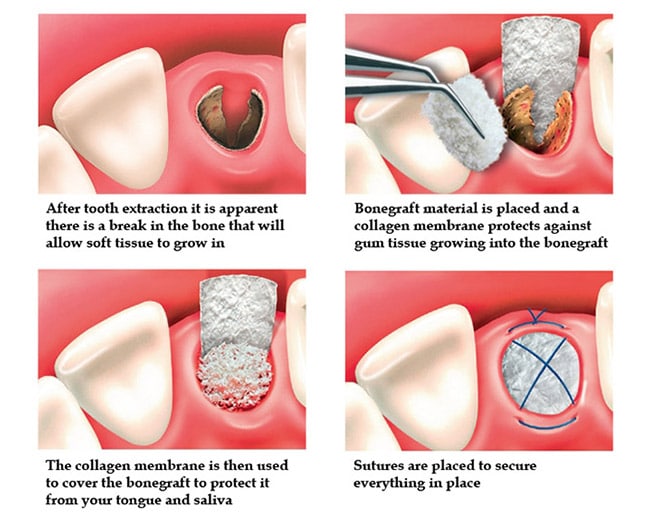
Ridge Preservation
Bone grafting techniques can sometimes be necessary to preserve the ridge of jawbone after a tooth has been extracted. This helps preserve height and width of the bone and allows for a better long term prognosis for restorative options, such as dental implants.
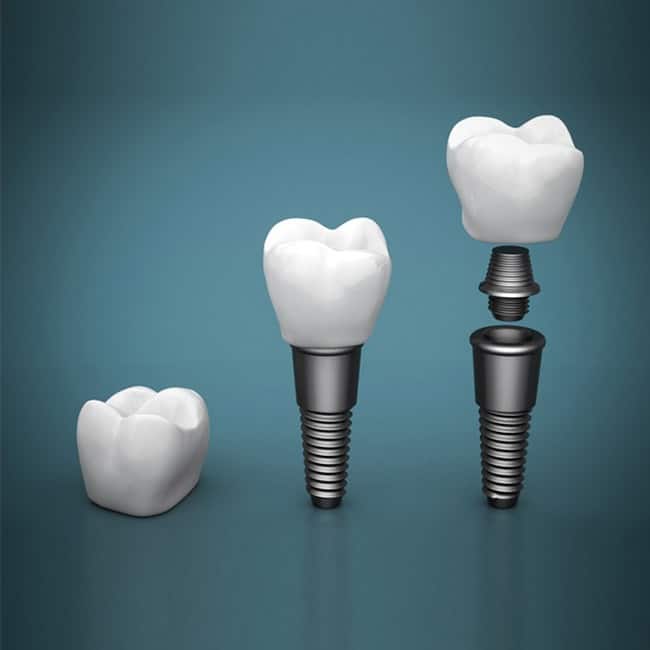
What is an Implant?
A dental implant is an excellent treatment for replacing missing teeth. A root form implant is the most common kind of dental implant. It is a small, titanium post that replaces the roots of a missing tooth, and is surgically positioned into the jawbone beneath the gum line that allows for replacement teeth or a bridge to be placed in that area.
How is an implant used?
An implant can support a variety of restorations, such as a single crown, multi-unit bridges, and full arch dentures. Some restorations, like a single crown and most bridges, are not removable. Other, like many full-arch dentures, can be removed for sleeping and cleaning.
Diagnosis and treatment
Depending on the situation, placing an implant involves several phases, and treatment times can widely vary. First we determine if an implant is right for you. We discuss your health history and treatment goals and perform a comprehensive examination to check the health of your gums and jawbone. We determine if you need any additional procedures, such as bone grafting or gum surgery.
To begin the procedure, a channel is shaped in the jawbone, and then the implant is placed into the prepared space. Sometimes a cover is placed onto the implant and the gums are stitched closed. This is called a two-stage procedure. In other cases that allow a single-stage procedure, an extension is attached to the implant at the time of surgery. At this point, it may be possible to place a temporary restoration. Over the course of the next few months, the implant will become securely fused to the bone. The last step is to attach your beautiful final restoration to the implant.
Restoring the implant with a crown
If the first phase included closing the gums over the implant, the second phase starts with surgical re-exposure of the implant. Another incision is made in your gums, and a small extension is placed to bring the implant above the gumline.
Then we start a process of creating the final crown. Though some of the steps might be different in your case, they usually include removing a temporary and taking impressions or a digital scan of your mouth.
The impression or digital scan of your mouth is used to make an accurate model of your mouth, including the implant. The model is used to create a custom crown that precisely fits the implant and your bite.
When your beautiful final crown is ready, we check the fit and your bite and then secure the crown to the implant.
The benefits of an implant
An implant has several benefits. Like the roots of natural teeth, it stimulates the jawbone when you chew. This preserves the jawbone and keeps it healthy. An implant is strong, comfortable, and secure. When the restoration is in place, the implant looks and feels much like natural teeth. An implant restored with a crown prevents the surrounding teeth from shifting into a space left by the missing tooth. Unlike replacing the tooth with a traditional bridge, there is no need to reduce the size of neighboring teeth. The crown with implant also looks and feels like your natural teeth when you chew and talk.
With careful homecare and regular checkups and cleanings here in our office, an implant can be an excellent long-term solution for missing teeth.
Call today for a consultation: 402.489.1262




